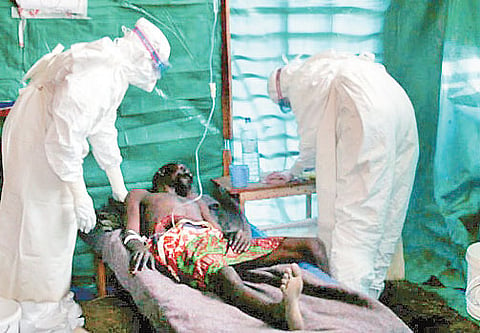

On New Year’s day in 1980, a Frenchman named Charles Monet who lived in a sugar plantation in Kenya in the shadow of Mount Elgna, decided to take a companion and camp on the fringes of the Elgon rain forest. Monet had arrived in Africa in the late seventies, when the HIV-AIDS epidemic was starting its global journey from Africa to become the terrifying new plague that would destroy lives—around 38 million so far—until retroviral therapy started to block the irreversible progression to death.
As Case Monet was to reveal, an even more terrifying virus noir was to emerge from the primeval African rainforests, whose very name, Ebola, strikes terror across the world. The current outbreak is the worst the world has ever seen and 2,127 cases have been reported so far. It all started with Patient Zero, a toddler, and spread from contact of his corpse with pall bearers. Airports are on viral alert, and any passenger traveling from or transiting through Ebola affected countries—Liberia, Sierra Leone and Guinea—is subjected to rigorous health checks. WHO has urged screening for passengers from these countries and Kenya has banned travellers from there.
Though no instances have been reported in India so far, the country remains vulnerable because of its importance as a major travel destination. The situation has worsened with many doctors unwilling to treat Ebola patients. Four Indian doctors—Yogesh Chandra, Dinesh Kumar, Hemant Jingar and Kapil Chouhan— said they were threatened to stay on duty at Primus Hospital in Nigeria. “No doctor would like to take a risk so high. Even though we pledge to treat every patient with our best ability and judgment, no doctor would voluntarily come forward to treat dangerous patients,” says a doctor from a leading government hospital in Delhi. There are two types of Ebola virus: Zaire and Sudan, whose kill rate is 9 out of 10.
Panic has spread among airline travellers after it was proved that air travel with an infected passenger aboard could infect others, by accidental contact. Richard Preston’s bestselling non-fiction thriller Hot Zone was the first authoritative book to be published on Ebola that traces its journey from Kitum Cave, where Monet was infected, in the rainforest to spread across Africa.
The cave, large enough to hold 70 elephants at a time, was in reality a petrified rainforest, a museum of prehistoric ghosts; of the skeletons and bones of ancestors of elephants, crocodiles and hippos frozen in the ceiling and the walls, and full of thousands of bats. Preston speculated that Monet pricked his hand on a crystal on the cave side or dipped his hand in a pool of bat guano.
Seven days later, Monet started getting a terrible headache. Nausea was followed by vomiting and high fever. His face looked paralytic, eyeballs frozen in their sockets, and his skin turned yellow and full of red spots. His personality changed, he became sullen and angry. His memory was affected. He was put on a plane to Nairobi for treatment and the Ebola virus had its maiden flight. Preston describes Monet’s symptoms appearing during the flight as truly frightening: he started coughing black speckled blood, his eyes had turned bloody and his skin was covered with bruises. His whole head was black and blue.
The connective tissue in his face had started to dissolve, his face appearing to detach itself from his skull. His vomit was black, brimming with Ebola virus. Inside him, his liver, kidneys, lungs, limbs and brain filled with blood clots. His nostrils were bleeding, and arterial blood was dripping all over his face and chin. At Nairobi Hospital, he went into shock, vomiting blood and his bloody intestines were expelled through his rectum. Blood was everywhere, infected blood, which at that time nobody knew bore the virus that needed just a touch of any part of the body that had sweat or a cut to infect. On the plane, Monet had handed the almost bursting sick bag to a flight stewardess. At Nairobi Hospital, black vomit and blood infected the doctor and nurses. They would all die.
That’s the thing about Ebola. It spares only a few, with death being the most likely way out. But, one woman who survived to tell the story, Gloria Tumwijuke—a middle aged midwife from Western Uganda who felt the chill of panic a few months back, while working in a local hospital in Kibaale, Western Uganda. A pregnant woman drenched in blood, painted everything red on her way to the emergency centre, right in front of her eyes. Gloria resolved to give her the best medical attention. As a parting gift, she received Ebola from her.
The bad news is that Ebola proves fatal for most. The good news is that Gloria wasn’t part of the majority. The epidemic is one of the most virulent viral diseases known to humankind, according to World Health Organisation. “If Ebola breaks out in India, it will be disastrous, as the country is not prepared to deal with such a lethal epidemic disease due to lack of health infrastructure, poor health facilities in rural areas, lack of availability of isolation beds in the country, lack of health awareness and lack of specialised centres. The fact that there is no definitive line of treatment and that vaccines are currently under development, it will take many lives if it breaks out here,” says Dr Prashant Saxena, Senior Consultant, Pulmonology, Critical Care and Sleep Medicine at Saket City Hospital.
In this daunting world of deadly infectious diseases, Ebola is just one. With reports of the recent outbreak in West Africa lasting over six months, Gloria is getting the jitters. Even though the present government has urged Najeeb Jung, Delhi’s Lt Governor to ensure health checks at the Indira Gandhi International Airport, it remains to be seen how effectively the country and the world will be able to manage this, and many other such life threatening viruses, spreading like wildfire.
The world, on the other hand, is witnessing an explosion of viruses that are Biosafety Level 4—which have no known cure, treatment or vaccines. The Marburg Virus (MARV), and Ravn Virus (RAVV) are frighteningly dangerous to humans because of their extreme ability to infect.
They kill almost all their victims. Extensively Drug-Resistant Tuberculosis (XDR TB) causes 40,000 cases a year in 49 countries and climbing. The very fact that this kind of Tuberculosis is resistant to most drugs, it leaves people suffering from it, completely on their own, to die a slow and painful death.
In fact, in some cases it’s been noted, that death doesn’t come instantly. The infection becomes progressively worse, causing each part of the body to collapse one by one. It leaves them gasping for air and soon, they don’t need it anymore. In 1998, a Nipah outbreak in Malaysia killed about 100 people. In Japan, 50,000 cases of Japanese Encephalitis, the main cause of viral encephalitis in Asia are reported annually, according to the Centers for Disease Control, and 30 per cent of those cases are fatal and another 30 per cent of patients are neurologically affected.
In 2010, a perfectly healthy girl of 11 years was hospitalised in Nevada because she complained of the usual headache, nausea, vomiting. Right upon admission, she showed abnormally high fever. In no time, she developed acute pulmonary edema, bradycardia and hypotension and was given mechanical ventilation. She had a dazed look about her and her eyes sunk deep into her sockets.
Her pupils became pale and dilated. Her brain functioning began to slow down as she developed Ventricular Tachycardia and subsequently passed away, just after five days of contracting Japanese Encephalitis. That’s how the disease bites into the body and consumes an individual completely.
Naegleria (brain-eating amoeba) is a swimmer’s risk—it is present in lakes and hotsprings, infiltrating the human body through the nose to reach the brain causing seizures, followed by a coma. The parasitic amoeba consumes brain matter causing death. Again in the year 2010, a case of a 7-year-old girl was reported. At first she only had mild headache, neck and abdominal pain. Once admitted to the intensive care unit, the situation only worsened. Her cerebrospinal fluid cell count and body chemistries showed abnormal results.
Her WBCs and RBCs started dropping. From here, she went downhill swiftly, as her seizures didn’t help the situation. She was advised endotracheal intubation and ventilation. Myoclonic jerks followed, decreasing her blood pressure. Her brain soon succumbed and her parents were left mourning her death. “The truth is that all of these viruses attack almost suddenly and without warning. The above are just a few. There are many more never-heard-before infections that medical sciences still don’t have solutions for. Nonetheless, they do surface every now and then. They sap the life out of you slowly and steadily, instead of killing you instantly,” says Gaurav Goel, a general physician with his own private practise in Mumbai.
Related closely to Ebola virus is another lethal virus called the Marburg virus. Both cause hemorrhagic fevers and in most cases, death comes knocking soon. The biggest jolt relating to Marburg is that it begins abruptly, debilitating your body with migraines.
Most patients develop haemorrhagic manifestations in the first week itself. That is followed by thin clotted blood, oozing out of one or various body parts. “Since these haven’t broken out in India yet, no hospital is equipped to deal with the symptoms.
It’s best to stop patients from arriving at our hospitals, as nothing much can be done to help him or her, which makes everybody feel vulnerable,” says a medical superintendent at Ram Manohar Lohia Hospital who was tending to the three Ebola-affected Nigerian patients being screened and tested at the hospital. Maarburg, like Ebola, is an African virus—a filovirus which resemble no other virus known to man. The fact that only one book and a few symposium papers exist on the virus shows how ill-prepared the world is to combat it if an epidemic occurs.
The biggest handicap pertaining to these infections, like Dr Goel points out, is the lack of knowledge regarding them. Marburg symptoms resemble Ebola’s—high fever, clotting and splashes of blood and then terminal shock. One out of four Marburg patients die, compared to yellow fever which claims only one in twenty.
The effects of Marburg are similar to rabies in the sense it destroys the brain. It affects the testicles and eyes: those who recover are wrecks of their former selves. Their hair would have fallen off, as well as skin from their faces, limbs and private parts. Medical scientists have identified the source as monkeys from Africa, like AIDS.
For instance, how many have heard of Cryptococcosis? The fungal infection that unfurled across western North America, last year, begins by attacking the lungs. Reportedly a third of the patients in the US died. Acute respiratory failure leaves an individual’s lungs quashed and dried.
“In the family of life-threatening infectious diseases, fungal infections are considered the worst. They often re-reappear after treatment. Because there are so many of such diseases, breaking out in different parts of the world all through the year, it’s making everybody more aware and scared at the same time. One should be happy, that for now, India isn’t grappling with many of these, as we still need years of research to devise effective treatment,” says an internal medicine doctor working at GB Pant Hospital in the city, who doesn’t want to be named.
Other lesser known contagions include Naegleria, a brain eating amoeba that finds its home in warm freshwater bodies like lakes, rock pits, mud puddles, untreated swimming pools and even soil. It’s harmless until it makes your nose its pathway to your brain while you swim. Once it attacks, an infection called Primary Amoebic Meningoencephalitis ruins the brain functions, proving fatal. Not too long ago, Naegleria claimed a life in Karachi, raising the recorded death toll to six. When nine-month-old Mahnoor, the daughter of a resident of Gulshan-e-Iqbal was taken to a hospital, she passed away in no time. Many cases go unreported because of misdiagnosis or medical ignorance. Even the ones that do get reported, often turn out to be fatal. In 2008, a man aged 30 was brought into Pakistan with uncontrollably high fever, cold sweats, palpitations, headache and seizures. He looked as if life has been sucked out of his body, leaving his jutting bones to expose his sorry state. With a dilated left eye. The treatment began, but the man passed away.
Then there are the hantaviruses that used to affect rodents until they migrated to humans. Infection used to happen when one came into contact with a rodent’s saliva or excrement. Recently, human-to-human transmission has also been recorded in Kerala and Andhra Pradesh. A few years ago, a 41-year-old Randolph County resident decided to spend some family time at a log cabin. Within a couple of days, he acquired fatigue, headache and fever which he ignored, thinking it’s the usual exhaustion or weather related common flu. When he started to get breathless, he was airlifted to a nearby hospital. There, he was put into incubation, with support of a high-frequency oscillator ventilator support. Subsequently the platelets in his blood plummeted dramatically. The levels of albumin in blood serum were reported abnormally low and there was renal insufficiency. After having bid farewell to his life of 41 years, he miraculously began to recover, over a month.
Bats have long been identified as carriers of deadly viruses. The Hendra Virus Disease and Nipah Virus Encephalitis are two. Nipah Virus, which is named after a Malaysian village where it was discovered first, has killed more than 252 since 1998. The fatality rate for Helminths Virus, that affect over a quarter of the world’s population, infect the intestinal tract, lungs, liver, skin or brain leaving the body dysfunctional. A person instantly freezes and dies. “Since the study and research in the area of many of these newly emerging and re-immerging infectious are still in progress, it will still take a few years to get on the better side of these diseases and be able to control, if not eradicate them,” says Dr Mudit Gupta, a private practitioner.
Medical science sees the emergence of these diseases as Earth fighting back. Many other rain forest agents are predicted to appear as a consequence of tropical biosphere devastation. The emerging viruses are surfacing from ecologically damaged parts of the earth. In a sense, the earth is mounting an immune response against human species. “The overall cure is to visualize public health as global ecological health. Man is not at the centre of web of world but a strand. If the rest of the web exists, man will,” says Dr Pankaj Aggarwal, MD. But till we don’t find a suitable antidote for such debilitating infections, people like Gloria and many others like her, continue to live in constant fear of a relapse.
Also Read: