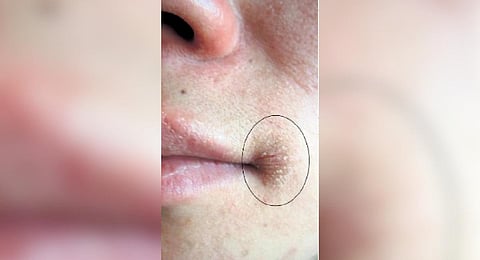

CHENNAI: An inflammatory skin disorder known as Angular Cheilitis frequently results in swollen, red patches near the corners of the mouth, either on one or both sides. This is typically not a serious situation, despite the agony. As a result, you are unable to eat, speak, or behave normally in front of people. Fortunately, there are treatments available that can help reduce inflammation and provide relief from the pain. It is important to seek medical advice and treatment to get back to a healthy smile.
Angular Cheilitis is also known as stomatitis and perleche. People frequently mistake this for herpes-related cold sores and attempt to cure it with coconut oil or cheese. Angular Cheilitis is not communicable, unlike cold sores.
Causes
Angular Cheilitis can affect people of any age, gender, or ethnicity. However, due to the high levels of drooling or salivation caused by many factors, this syndrome is frequently seen in children and older adults. Our saliva contains specific enzymes that help break down our food. Dryness is brought on by saliva that has gathered in the corners of the mouth, and this dryness can eventually cause the skin to crack open, resulting in Angular Cheilitis.
Other causes of Cheilitis include nutritional inadequacies, iron shortage, snoring while sleeping, crooked teeth, atopic dermatitis, thumb sucking, smoking, stress, and face mask use. On rare occasions, bacteria or fungus that enter the crack cause infection or inflammation.
Symptoms
Sores at mouth and lip corners are the typical symptoms. The additional signs and symptoms are:
Contact a medical professional if any of the symptoms are present or if they are new, severe, or persistent.
Diagnosis
After a reliable source of treatment is ineffective, your family doctor or a dermatologist can diagnose Angular Cheilitis by taking a mouth swab to test for viruses like herpes or any fungal infections. In addition to examining your lifestyle, health history, and symptoms, they may also perform blood tests to look for any nutritional deficiencies.
Treatment
The underlying causes of Angular Cheilitis will determine the course of treatment. The lack of nutrients such as protein, iron, or B vitamins is the cause of the issue, the expert may suggest taking dietary supplements to resolve it.
If a fungus is to blame, antifungal medication will be given to apply topically on the affected area of your mouth. If bacterial infection is the reason, the specialist will probably suggest a topical antibiotic cream or ointment.
Topical antiseptics are one more alternative for the treatment of mouth sores along with topical steroid cream and injections of filler to lessen mouth cracks.
Prevention
Preventing Angular Cheilitis can be done with good hygiene and stringent skin care. You can lessen the possibility of infections developing by keeping the area surrounding your mouth moisturized and irritation-free. To prevent saliva buildup at the corners of your mouth, you can also use petroleum jelly or coconut oil.
The following guidelines can help lower the risk of Angular Cheilitis.
(The writer is a dermatologist at Fortis Malar Hospital, Adyar)